홈 > 연구소 > 논문 / 학술활동
연구소
마마파파&베이비의 핵심인 베이비 드림 난임 연구소는
그간의 연구학술 성과에 안주하지 않고,
늘 한계를 뛰어넘기 위해 노력합니다.
연속 배아 채점 시스템은 Time-lapse 모니터링 시스템 대신 사용할 수 있습니다.
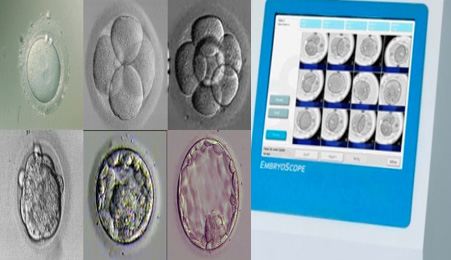
2016년 미국불임학회(ASRM) P-263 Sequential embryo scoring system can substitute for Time-lapse monitoring system (연속 배아 채점 시스템은 Time-lapse 모니터링 시스템 대신 사용할 수 있습니다. )
Y. Kim,a H. Sun,b H. Chi,a S. Kim,a K. Lee,b S. Kwak,a J. Park,a C. Yoo,a J. Kim.b
aBabydream Research Center, Mamapapa & Baby OBGY Clinic, Ulsan, Korea, Republic of;
bMamapapa & Baby OBGY Clinic, Ulsan, Korea, Republic of.
DESIGN
All fresh, non-donor IVF cycles performed from January 2015 through August 2015 (n=485). After insemination, embryos were scored at the following 3 time points: 2-cell cleavage (26h), day 2 (40-41h), and day 3 (64-65h). The highest score of the embryo at 3 time points is as follows: 2-cell cleavage (2 points) + day 2 (5 points) + day 3 (5 points) = 12 points. In two embryos transfer, the highest total score is 24 points.
MATERIALS AND METHODS
The score was dependent on three factors: (number of blastomere, synchrony of cleavage, level of fragmentation). Scoring was done by subtracting scores from embryos with one or more defects. To determine a cut-off value, pregnancy rate was evaluated in one point unit from 6 points to 24 points based on two embryos transfer. Based on the cut-off value, embryos were divided into two groups, and the pregnancy and implantation rate were checked.
RESULTS
The cut-off value was 16 points, and it was confirmed that pregnancy rate significantly improved. When the two groups (group (1) scored higher than 16 points, group (2) scored less than 15 points) based on the cut-off value were divided and compared. Patient characteristics were similar in the 2 groups. In each group, age (Group 1: 35.6±2.0 vs. Group 2: 36.0±1.9) basal AMH conc. (4.2±2.9 vs. 4.8±2.8ng/ml), and endometrial thickness (10.2±2.2 vs. 10.1±2.0mm) did not show significant differences. There were no significant differences between 2 groups in the number of MII oocytes (10.6±6.0 vs. 10.6±5.3) and number of embryo transfer (2.0±0.1 vs. 2.0±0.1). Group (1) had a significantly high pregnancy rate (68.8%, P<0.001) and implantation rate (57.1%, P<0.001) compared to that of Group (2) (41.6% and 31.6%, respectively).
CONCLUSIONS
Our study evaluated the continuous development process of the embryo through the sequential embryo scoring system. We found that embryos with scores higher than 16 points resulted in a significantly high pregnancy rate. Therefore, the sequential embryo scoring system is effective in predicting high pregnancy rates.
-
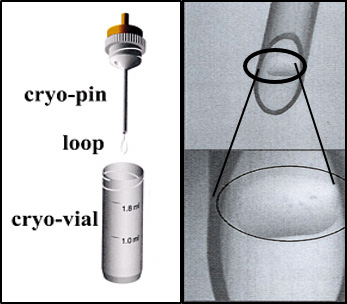 2017년 유럽불임학회(ESHRE) P-
Cryo-loop와 Hemi-straw를 이용한 인간 배아 유리화 동결에서 해동 후 손상되지 않은 배아와 임상 결과의 비교.
2017년 유럽불임학회(ESHRE) P-
Cryo-loop와 Hemi-straw를 이용한 인간 배아 유리화 동결에서 해동 후 손상되지 않은 배아와 임상 결과의 비교.
-
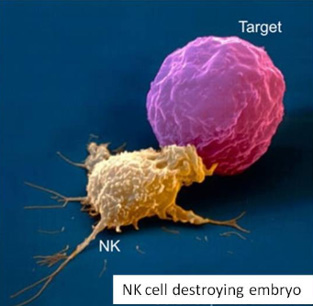 2016년 미국불임학회(ASRM) P-595
반복착상 실패 환자 에서 면역치료요법이 유용할 것인가; 특히 높은 자연살해세포를 가진 환자에서?
2016년 미국불임학회(ASRM) P-595
반복착상 실패 환자 에서 면역치료요법이 유용할 것인가; 특히 높은 자연살해세포를 가진 환자에서?
-
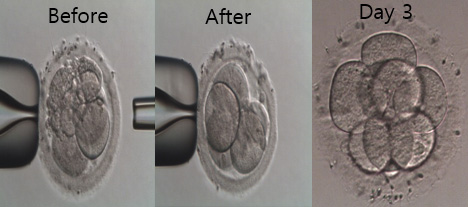 2016년 미국불임학회(ASRM) P-555
2일 째 파편화된 인간 배아에서 파편제거는 순차적 배아의 발달과 임상적 결과를 유의하게 증가시킨다.
2016년 미국불임학회(ASRM) P-555
2일 째 파편화된 인간 배아에서 파편제거는 순차적 배아의 발달과 임상적 결과를 유의하게 증가시킨다.
-
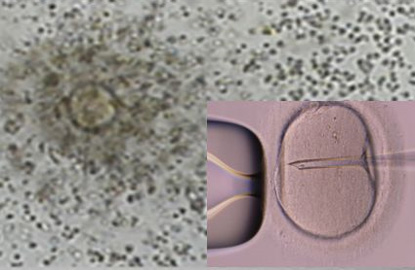 2016년 미국불임학회(ASRM) P-317
정자 DNA 파편화 지수가 높은 환자에서 ICSI가 전통적인 IVF에 비해 임신율을 유의하게 증가시켰다.
2016년 미국불임학회(ASRM) P-317
정자 DNA 파편화 지수가 높은 환자에서 ICSI가 전통적인 IVF에 비해 임신율을 유의하게 증가시켰다.
-
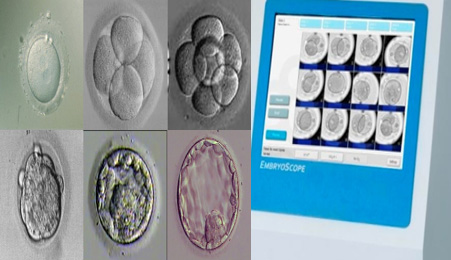 2016년 미국불임학회(ASRM) P-263
연속 배아 채점 시스템은 Time-lapse 모니터링 시스템 대신 사용할 수 있습니다.
2016년 미국불임학회(ASRM) P-263
연속 배아 채점 시스템은 Time-lapse 모니터링 시스템 대신 사용할 수 있습니다.
-
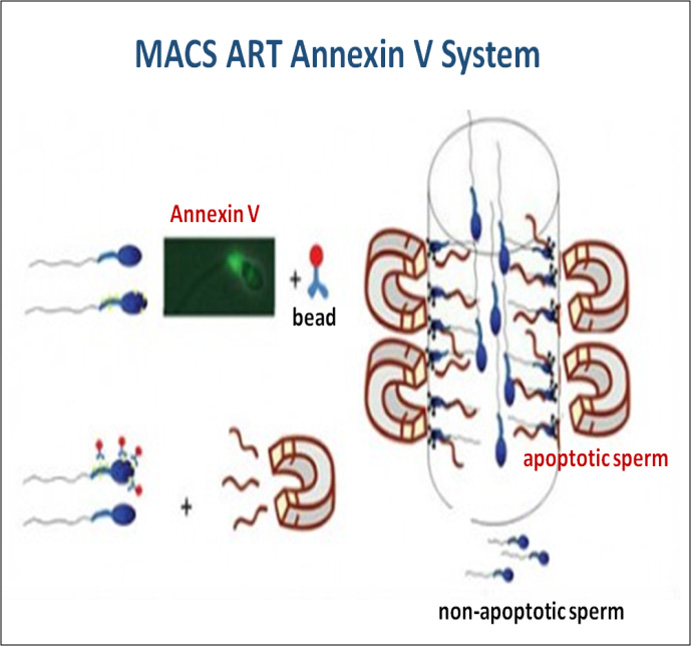 2016년 유럽불임학회(ESHRE) P-021
중층원심분리와 자석활성화세포분리 방법의 병용은 정액샘플의 정자 DNA손상지수를 유의하게 감소시킨다.
2016년 유럽불임학회(ESHRE) P-021
중층원심분리와 자석활성화세포분리 방법의 병용은 정액샘플의 정자 DNA손상지수를 유의하게 감소시킨다.
-
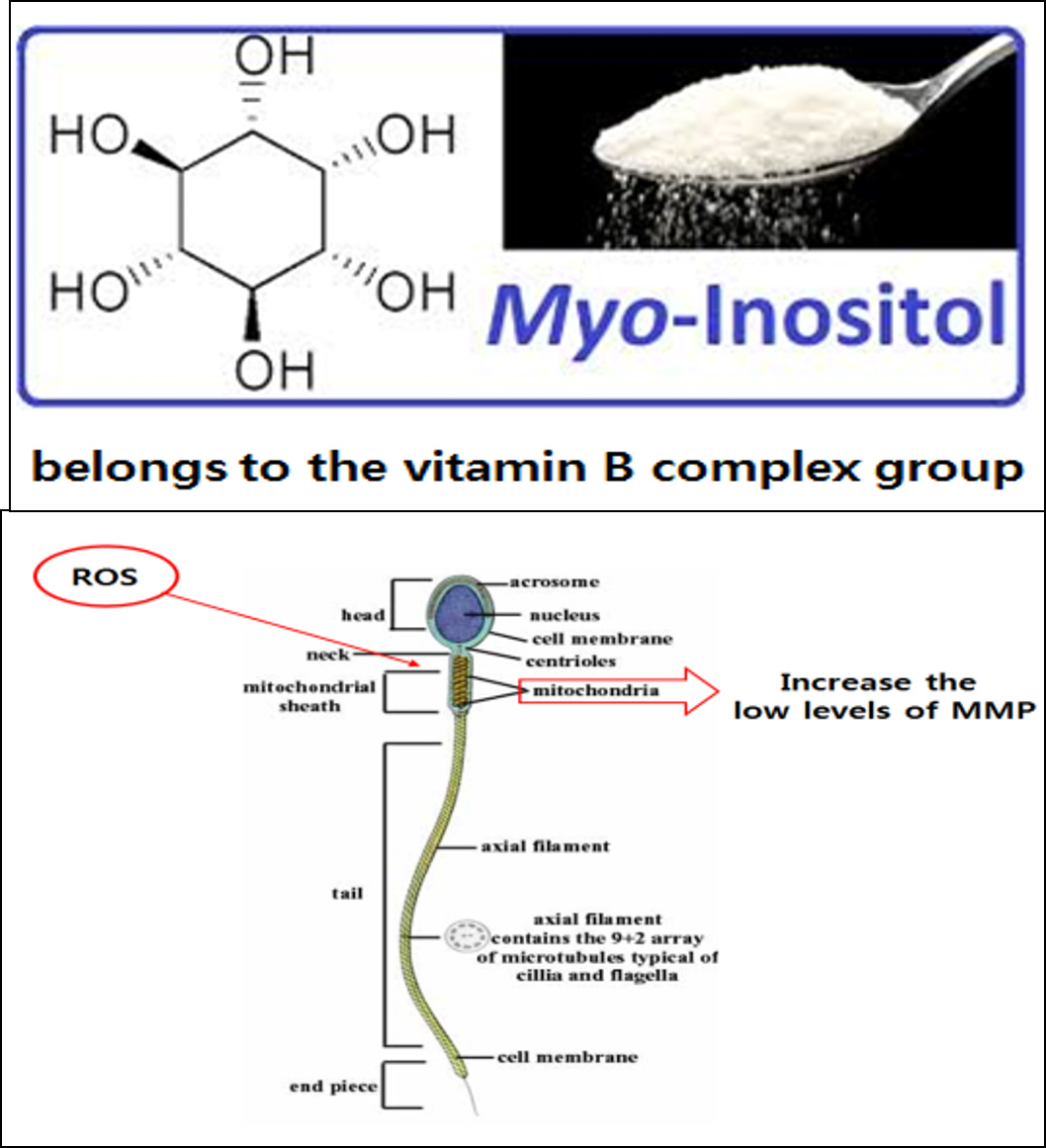 2016년 유럽불임학회(ESHRE) P-022
정액처리 배양액에 Myoinositol의 첨가는 무력정자증 환자의 인공수정시술 시 정자의 운동성과 임신율을 향상시켰다.
2016년 유럽불임학회(ESHRE) P-022
정액처리 배양액에 Myoinositol의 첨가는 무력정자증 환자의 인공수정시술 시 정자의 운동성과 임신율을 향상시켰다.
-
 2016년 유럽불임학회(ESHRE) P-182
다낭성난소증후군 환자의 동결융해배아 이식을 위한 효율적이고 환자친화적인 자궁내막 준비방법; letrozole을 이용한 배란유도
2016년 유럽불임학회(ESHRE) P-182
다낭성난소증후군 환자의 동결융해배아 이식을 위한 효율적이고 환자친화적인 자궁내막 준비방법; letrozole을 이용한 배란유도
